Yes, port wine stains can grow larger over time, but that's only part of the story. That said, some people wonder can bacteria grow on ice, but growth and survival depend on temperature and conditions. Bacteria can grow on wood cutting boards if they are used for food and not cleaned and dried properly bacteria grow. What's more common than actual enlargement is that they darken from pink or red to a deeper purple, thicken, and eventually develop raised bumps or nodules as you age. Both things can happen simultaneously, and understanding which is occurring matters a lot for deciding what to do next.
Do Port Wine Stains Grow? What Changes Over Time
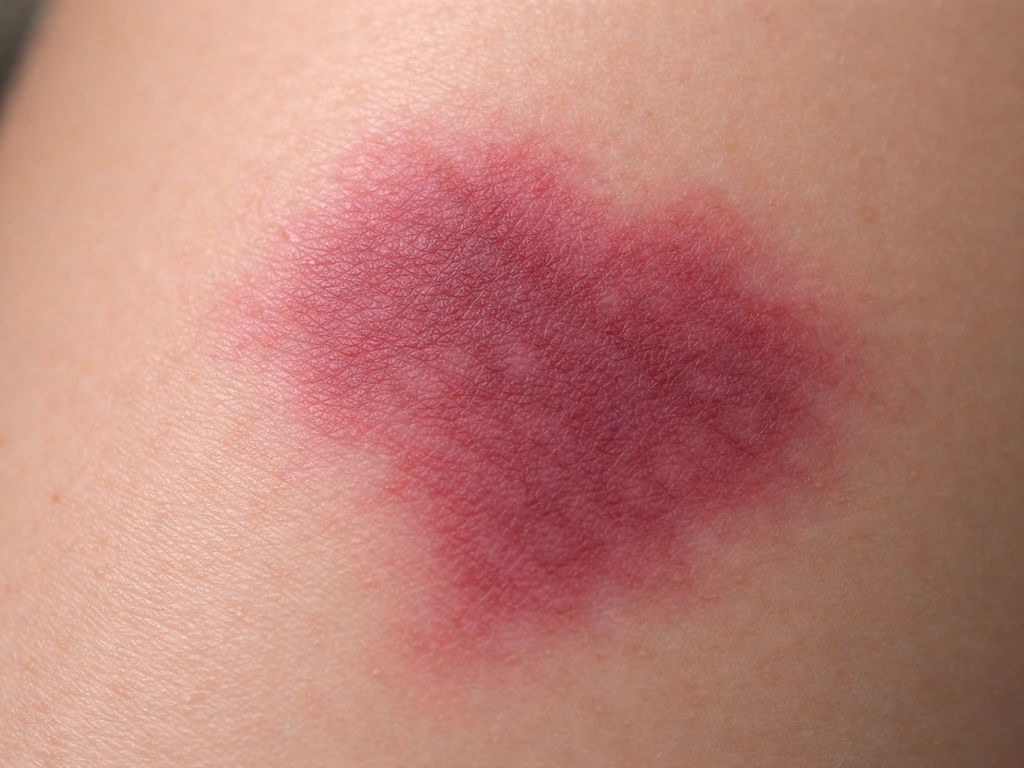
What port wine stains actually are (and why they change)
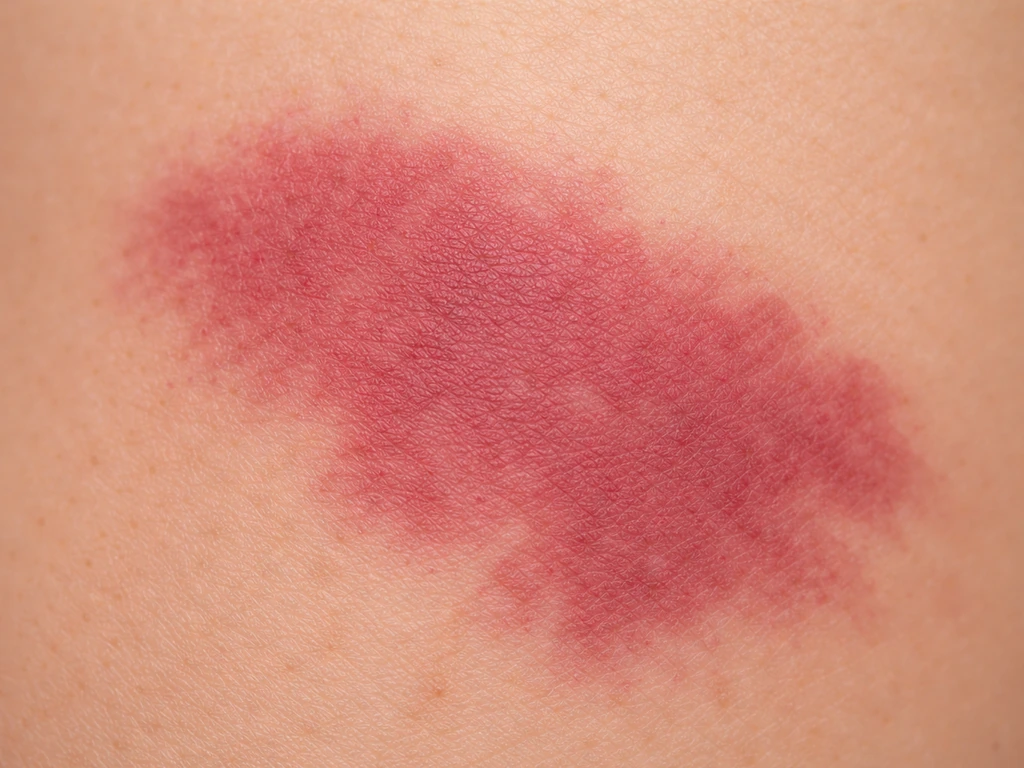
A port wine stain (PWS) is a congenital vascular malformation, not a bruise or a rash. It forms before birth when the tiny capillaries and post-capillary venules in a patch of skin fail to develop normal nerve control. Without proper neural regulation, those vessels gradually dilate over time, a process called ectasia. The skin in that area has a measurably reduced nerve density and an increased vessel-to-nerve ratio compared with normal skin, and that imbalance is essentially what drives the progressive changes you see.
They show up at birth as flat, pink or red patches with well-defined borders. They are not tumors and they are not infections. But they are classified as progressive diseases, meaning the underlying pathology continues to evolve across a lifetime, not just in childhood.
Do they actually grow, or just look worse?
Both, depending on the person and the stage of life. Some port wine stains remain essentially unchanged for years or even decades. But many do not. Research involving over 400 patients found that roughly 65% showed hypertrophy (thickening) or nodularity by their fifth decade, with the average age of hypertrophy appearing around 37 years. Separately, a large cohort study found hypertrophy in about 20% of patients overall, rising to 71% of patients over age 50.
So the most accurate answer is: true enlargement in surface area can happen, but the more consistent and universal change is darkening and thickening. A stain that started as a faint pink patch can, over 20 to 30 years, become a deep purple, raised, cobblestone-textured patch that bleeds more easily. That is not cosmetic drift. That is a documented biological progression driven by progressive vascular ectasia.
Normal progression vs. something to act on quickly
Not every change in a port wine stain is alarming. Gradual darkening from pink to red to purple over years is typical. Slow thickening that develops into a slightly raised, rougher texture in your 30s or 40s is also within the expected range. These changes are frustrating, but they are the known natural history of the condition.
What warrants a faster call to a dermatologist is a different set of changes: rapid enlargement over weeks to months, sudden bleeding from blebs or nodules that was not present before, or any change that feels disproportionately fast relative to your age and the stain's prior history. These can sometimes indicate a secondary vascular change that needs evaluation.
The most urgent situation is a port wine stain on or near the face, particularly around the forehead, upper eyelid, or along the distribution of the trigeminal nerve. A facial PWS in that location is a recognized marker for Sturge-Weber syndrome, a neurocutaneous condition that involves deeper tissue abnormalities. About 98% of people with Sturge-Weber syndrome have a facial port wine stain, and roughly 60% develop glaucoma. If a child or adult has a PWS in that zone and has never had a formal evaluation, an ophthalmology appointment and brain MRI are genuinely important, not optional.
Factors that can make it look like it's growing faster
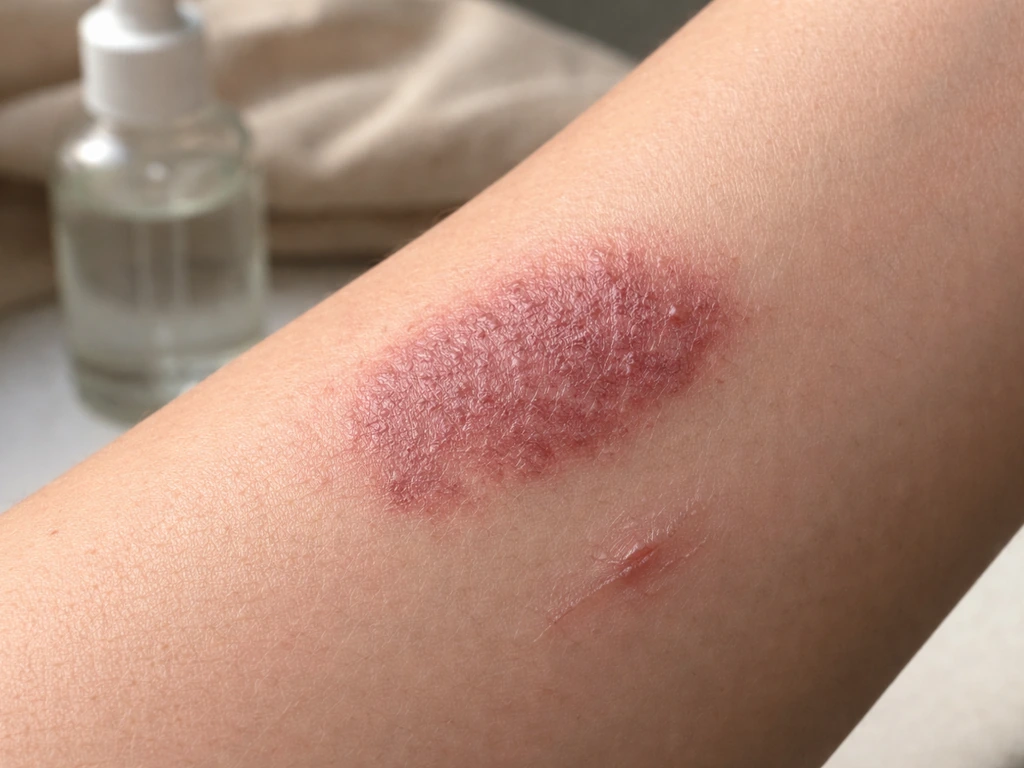
Several external and internal factors can accelerate or amplify the visible changes in a port wine stain, even if the underlying vascular malformation is not expanding in area.
- Sun exposure: UV damage thickens and changes the overlying skin, which can make a stain look darker and more prominent. Unprotected sun exposure is one of the most controllable factors in how quickly the appearance worsens.
- Hormonal changes: Pregnancy and puberty are both associated with increased vasodilation throughout the body. Port wine stains can appear more flushed or slightly more prominent during these periods.
- Trauma or injury to the area: Physical injury to skin over a port wine stain can trigger localized vascular changes and make the area look worse temporarily or permanently.
- Age-related skin thinning: As the skin above the stain thins with age, the underlying dilated vessels become more visible, which reads visually as darkening even without new vascular growth.
- Heat and alcohol: Both cause temporary vasodilation that can make the stain look more vivid, though this is reversible.
Unlike the environmental conditions that affect microbial growth (temperature, moisture, pH, and so on), the factors driving port wine stain progression are primarily biological and vascular. Because bacteria can grow in soda under the right conditions, it helps to understand how microbes respond to things like moisture and pH can bacteria grow in soda. In contrast, whether can bacteria grow on copper depends on the metal surface and conditions, but copper is generally considered antimicrobial. Can bacteria grow in water bottles is a related question about how moisture and temperature can help microbes multiply in the right conditions microbial growth. You cannot starve the progression by changing an external substrate. This is also why bacteria struggle to grow on copper pennies, since copper ions can disrupt microbial cells why bacteria will not grow on copper pennies. But you can slow the visible worsening by controlling sun exposure and seeking treatment early. If you are trying to manage skin-related staining or irritation at home, it can also help to understand that can bacteria grow on linen under certain conditions.
Treatment options that slow or limit progression
The most effective and best-studied treatment for port wine stains is pulsed dye laser (PDL) therapy. The 585 to 595 nm wavelength range has the strongest clinical track record for safety and effectiveness. PDL targets oxyhemoglobin in the dilated vessels, destroying them while minimizing damage to surrounding skin. Treatment is typically done in multiple sessions spaced about 4 to 8 weeks apart (some research suggests a 2-week interval may produce greater lightening with good tolerability). Side effects are mainly purpura (bruising-like discoloration) and swelling that generally resolve within about two weeks.
For more advanced stains with developed nodules or blebs, longer-wavelength lasers like Nd:YAG (1064 nm) are sometimes used alongside PDL because they penetrate deeper. The tradeoff is that longer wavelengths have a higher adverse event profile, including a greater risk of pigmentary changes and scarring, because the deeper penetration requires higher fluences and hemoglobin absorption is weaker at those wavelengths.
One realistic expectation worth setting: treatment lightens the stain but rarely eliminates it entirely, and maintenance sessions are usually needed after several years because the stain can darken again. Getting treatment early in life, before significant thickening or nodularity develops, generally produces better outcomes and requires fewer sessions.
| Treatment | Best For | Typical Outcome | Key Risk |
|---|---|---|---|
| Pulsed Dye Laser (PDL) 585-595 nm | Flat or mildly thickened stains, all ages | Significant lightening over multiple sessions | Purpura, rare blistering if dose too high |
| Nd:YAG (1064 nm) | Deep or nodular/blebbed stains | Targets deeper vessels, used with PDL | Higher risk of pigment changes and scarring |
| Alexandrite / IPL | Alternative when PDL is insufficient | Variable; second-line option | Pigmentary changes, less studied for PWS |
| No treatment | Stable, unchanged stains in low-risk locations | Progressive darkening and thickening likely over decades | Ongoing natural progression |
Getting the right diagnosis and knowing when to see a specialist
Port wine stains are almost always diagnosed clinically, meaning a dermatologist can usually confirm the diagnosis by looking at the stain, noting its history since birth, and observing its typical features. No biopsy or lab work is needed in straightforward cases.
The picture changes when associated syndromes are possible. If the port wine stain is on the face, especially the forehead or upper eyelid, a referral to ophthalmology is important to screen for glaucoma, which can appear even in early childhood. Patients with forehead involvement should also have a brain MRI to check for leptomeningeal involvement consistent with Sturge-Weber syndrome. These evaluations are not routine for all port wine stains, only for those in at-risk anatomical locations.
Here is a practical summary of when to make an appointment and how urgently:
- Facial PWS involving the forehead, upper eyelid, or trigeminal nerve distribution: Schedule an ophthalmology evaluation and discuss brain MRI with your doctor soon, even if the stain looks stable.
- Rapid enlargement or change over weeks to months: See a dermatologist within a few weeks, not months.
- Newly developing nodules or blebs that bleed: Book a dermatology appointment to assess and discuss laser options for the affected area.
- Gradual darkening or thickening over years with no facial involvement: This is expected progression. Schedule a consultation with a dermatologist experienced in vascular lasers to discuss starting PDL treatment before the stain becomes harder to treat.
- No changes noticed, stain on trunk or limb: Still worth a single dermatology review to establish a baseline and get advice on sun protection and monitoring.
The bottom line: port wine stains do grow and change, and doing nothing tends to lead to a worse outcome over time. If you are wondering about hygiene instead, a common question is whether loofahs grow bacteria do loofahs grow bacteria. Early laser treatment, consistent sun protection, and the right specialist evaluation based on location give you the most control over how this progresses.
FAQ
If my port wine stain seems bigger, how can I tell whether it is true enlargement versus just becoming darker and thicker?
True enlargement means the patch expands its boundary area on the skin. Darkening and thickening can make a stain look wider even if the border stays the same. A helpful check is to take dated photos with the same lighting and measure the visible border periodically, for example every 3 to 6 months, and compare whether the edge actually moves.
Can port wine stains suddenly change or worsen quickly, or is it always gradual?
Most changes are slow over years, but some people notice faster shifts. Rapid growth over weeks to months, new bleeding from previously stable bumps, or a noticeable acceleration compared with your prior pattern should prompt an urgent dermatology visit to rule out secondary vascular changes.
Do port wine stains grow more in childhood, or can they keep progressing well into adulthood?
They can progress across a lifetime. Many people see the clearest evolution in early decades, but hypertrophy and nodularity are still documented in later adulthood, especially after age 50. That means treatment planning and follow-up should not stop after adolescence.
Does sun exposure affect port wine stain progression, and what is a practical sun-protection plan?
Sun exposure can make the skin changes more visible and can contribute to worsening appearance. A practical plan is daily broad-spectrum sunscreen on exposed areas, protective clothing (hat and sleeves when relevant), and minimizing intense midday sun, since early light exposure tends to matter most for long-term visibility.
Will antibiotics, topical creams, or hygiene changes stop a port wine stain from growing?
Port wine stains are vascular malformations, not infections, so antimicrobial or hygiene steps do not target the underlying process. The biggest evidence-based options are laser treatment and appropriate specialist evaluation when indicated by location.
If the lesion bleeds when it gets raised, does that mean it is cancer or an infection?
Bleeding can occur when ectatic vessels become more superficial due to thickening and nodules. It does not automatically mean cancer or infection. However, any bleeding that is new, persistent, or accompanied by rapid change deserves prompt assessment by a dermatologist.
How do I know whether my port wine stain location requires an eye and brain evaluation?
If the stain is on or near the face, particularly the forehead or upper eyelid, it can be a marker for Sturge-Weber syndrome. In that situation, an ophthalmology evaluation for glaucoma screening and, when the forehead is involved, a brain MRI are typically considered appropriate rather than waiting for symptoms.
At what age should someone start pulsed dye laser treatment for the best results?
Earlier treatment is generally associated with better cosmetic outcomes, especially before substantial thickening or nodularity develops. That said, adults can still improve, so the key decision is whether there is treatable vessel ectasia and whether the lesion has evolved, which your dermatologist can evaluate.
If I do pulsed dye laser, will the stain disappear completely and stay away?
Complete elimination is uncommon. Even when there is substantial lightening, the stain can darken again later, so maintenance sessions are often needed after several years. Your treatment plan should include realistic long-term expectations, not just a single course.
What are the most common side effects of pulsed dye laser, and how long should I expect them to last?
The most typical immediate effect is purpura, a bruise-like discoloration, along with swelling. These usually resolve within about two weeks. Your clinician may also provide specific aftercare advice to reduce irritation and optimize lightening.
If my stain is thicker with nodules, will the standard laser still work?
Standard pulsed dye laser is still commonly used, but deeper involvement may require additional or different wavelengths. Longer-wavelength lasers like Nd:YAG can penetrate deeper for more advanced lesions, but they have a higher risk of pigmentary changes and scarring, so a careful risk-benefit discussion is important.
Is biopsy ever needed to diagnose a port wine stain or to investigate changes?
In typical cases, diagnosis is usually clinical based on appearance and history from birth, so biopsy is generally not needed. Biopsy or lab work is more likely only if the presentation is atypical or the changes raise concern for another condition.
Can Bacteria Grow on Copper? Survival vs Growth Explained
Yes, bacteria can survive on copper but usually do not grow; explains conditions that affect survival and practical sani


