Staphylococci are pus-forming bacteria that grow in a surprisingly wide range of conditions, from warm human skin and moist nasal passages to room-temperature food left on a counter. If you are trying to understand where these bacteria actually live and multiply, and what that means for preventing contamination or infection, this guide walks through all of it in plain terms.
Staphylococci Are Pus-Forming Bacteria That Grow in What
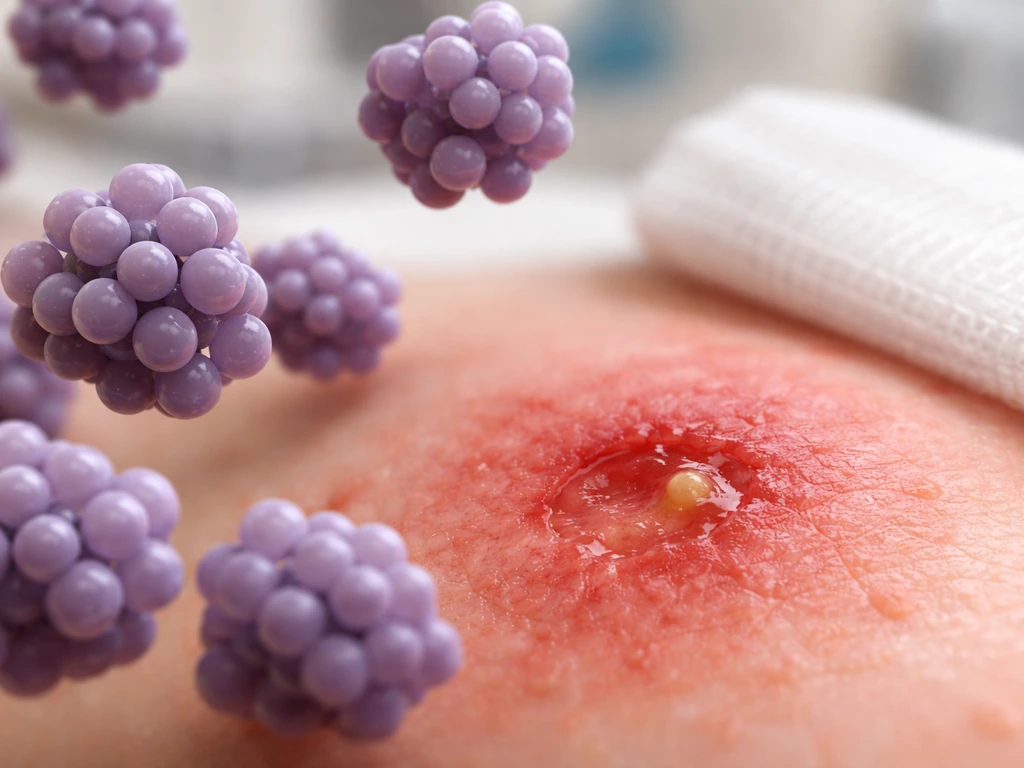
What 'pus-forming' actually means
Staphylococci are a large group of bacteria, and the ones most relevant to human health are the ones that produce virulence factors capable of causing tissue damage. Staphylococcus aureus is the main pus-forming species. The 'pus' part is not just a gross side effect. It is a direct result of what these bacteria do to your immune cells. S. aureus produces toxins called leukocidins that kill white blood cells. When white blood cells rush to fight the infection and are killed in large numbers, the resulting debris, dead cells, and fluid become the thick yellowish material we call pus.
The hallmark of a staphylococcal infection is an abscess: a walled-off pocket with a fibrin shell and a central core of pus containing both bacteria and dead leukocytes. Boils (furuncles) are one of the most familiar examples. A wound or skin lesion with a white or yellow center, or one that drains thick fluid, is consistent with a staphylococcal infection. That signature look is useful because it tells you something about what organism you are likely dealing with before any lab test is run.
Not all staphylococci behave this way. Coagulase-negative staphylococci (like S. epidermidis) are far less aggressive and rarely cause the classic abscess picture. When people talk about 'pus-forming' staphylococci, they are almost always referring to S. aureus, the coagulase-positive species. Understanding pus-forming bacteria that grow in bunches or clusters helps clarify which specific organisms fall into this category and why their arrangement under a microscope matters for identification.
Where staphylococci naturally live on and in the body
About one in three people carries S. aureus in their nose right now, usually without any illness at all. The anterior nares (the front of the nostrils) are the primary reservoir. Studies put nasal carriage rates anywhere from 20% to 80% depending on the population, but the most commonly cited figure is around 20 to 40%. That means if you are in a room with ten people, two to four of them are quietly hosting S. aureus in their nasal passages.
Beyond the nose, S. aureus colonizes skin, particularly in moist, warm areas like the armpits, groin, and perineum. Coagulase-negative staphylococci, especially S. epidermidis, favor similar spots: axillae, groin, toe webs, and even the conjunctiva of the eye. These bacteria are not invaders in the usual sense. They are part of the normal human flora. The problem starts when the skin barrier breaks (a cut, a needle, a surgical incision) and they get access to deeper tissue.
Mucous membranes are another key habitat. The moist lining of the nasal passages, throat, and vaginal tract can all carry staphylococci without obvious infection. This is why nasal carriage is considered a major risk factor for subsequent S. aureus infection, especially in surgical patients or people with compromised immune systems.
The environmental conditions that let staphylococci thrive
Temperature

S. aureus is a genuinely flexible organism when it comes to temperature. It can grow anywhere from about 7°C (45°F) up to 48°C (118°F), with an optimum right around 37°C (98.6°F), which is exactly human body temperature. That is not a coincidence. This range also explains why food left at room temperature (roughly 20 to 25°C) is a real concern. Enterotoxin production has its own temperature window, roughly 10°C to 46°C, so food sitting in the classic 'danger zone' of 40°F to 140°F (4°C to 60°C) is a setup for both bacterial growth and toxin accumulation.
pH tolerance
S. aureus can grow across a pH range of roughly 4.5 to 9.3, with an optimum near neutral (pH 7.0 to 7.5). This is a relatively broad tolerance. It means slightly acidic foods are not automatically safe from staphylococcal growth, though very acidic environments (below pH 4.5) do reliably inhibit it. When formulating or storing foods with mild acidity, pH alone cannot be counted on to stop growth unless it is well below 4.5.
Moisture and water activity
Water activity (aw) is the measure of available water in a food or environment. S. aureus is notably tolerant of low-moisture conditions compared to many other pathogens. It can grow at water activity values as low as around 0.86 to 0.87 under favorable temperature and pH conditions, though growth is much more robust closer to aw 0.99. This low-moisture tolerance is one of the reasons staphylococci can persist in salt-cured meats, dried foods, and on drying skin surfaces better than organisms like Salmonella.
Oxygen needs
S. aureus is a facultative anaerobe. That means it grows faster and more efficiently when oxygen is present, but it does not need oxygen to survive and multiply. In anaerobic conditions (inside wounds, within biofilms, under food packaging, in crevices on surfaces), it still grows, just more slowly. Research also shows that anaerobic conditions actually stimulate expression of biofilm-associated genes in staphylococci, which has real practical implications for how persistent these bacteria can be in oxygen-limited environments.
What surfaces and substrates they actually colonize
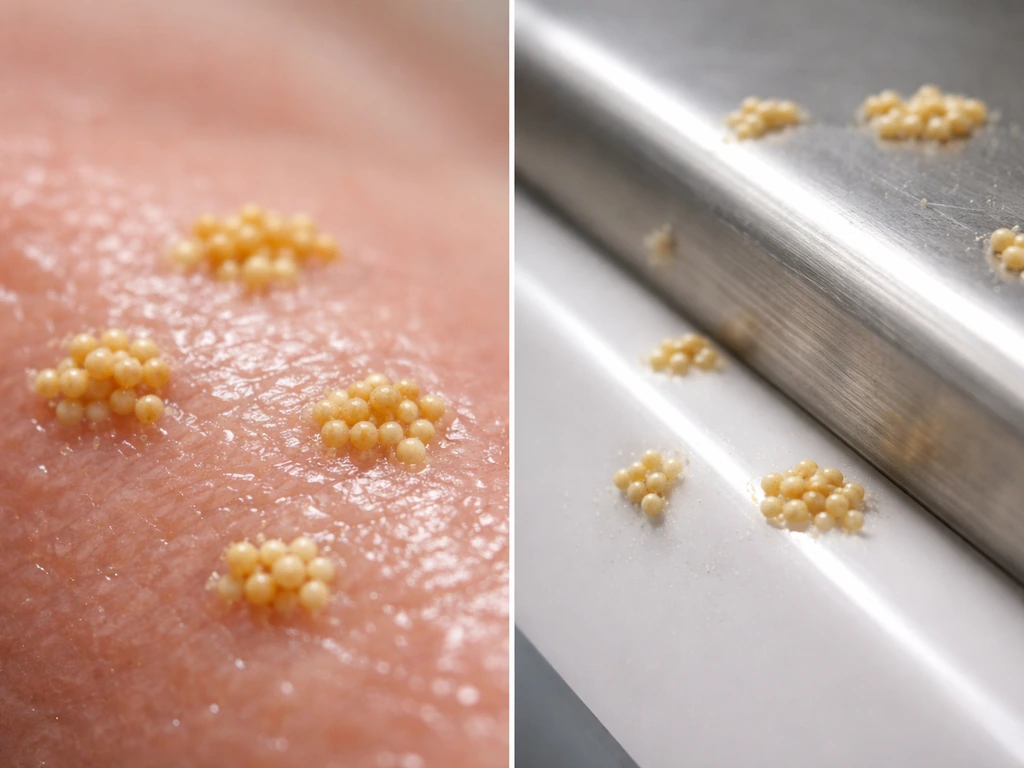
In clinical and food settings, staphylococci do not limit themselves to living tissue. They colonize a wide range of surfaces, both biological and non-biological (abiotic). On the biological side: skin, wound surfaces, mucous membranes, and the surfaces of implanted medical devices coated with host proteins. On the abiotic side: glass, metals, and plastics can all become colonization sites once a thin layer of host proteins (fibronectin, fibrinogen) adsorbs onto the surface, giving the bacteria something to attach to.
In food environments, the relevant substrates are protein-rich foods at room temperature: sliced deli meats, egg salad, cream-filled pastries, potato salads with mayonnaise, and cooked poultry held warm. These are not just theoretically risky. They are the foods that appear repeatedly in documented outbreak reports because they provide the nutrients, moisture, and temperature that S. aureus needs to multiply and produce enterotoxin.
In healthcare settings, high-touch surfaces are the key concern: bed rails, faucet handles, doorknobs, and call buttons. Contaminated hands touching these surfaces and then touching patients or food create a reliable chain of transmission. This is the same logic behind the focus on hand hygiene in both hospital and food service settings.
How they survive and persist (biofilms, drying, and cleaning)
One of the more important things to understand about staphylococci is that they are not fragile. They form biofilms, which are structured communities of bacteria embedded in a self-produced matrix that makes them far harder to kill than free-floating (planktonic) cells. Where biofilms grow matters a great deal in practice: they show up on medical device surfaces, food processing equipment, and anywhere bacteria can attach and colonize without being regularly disrupted.
S. aureus can also form dry-surface biofilms on environmental surfaces, and these dry biofilms are actually more resistant to heat treatment than traditional moist biofilms. That matters in food processing plants and healthcare facilities where heat-based cleaning or pasteurization is part of the protocol. A biofilm that has dried onto stainless steel or plastic can survive conditions that would easily kill planktonic cells.
For cleaning and disinfection to actually work, the disinfectant needs to stay wet on the surface for the full contact time listed on the product label. This is consistently where cleaning protocols fail in practice. Someone sprays a surface, wipes it immediately, and considers it clean. But if the product requires a two-minute dwell time and was wiped after ten seconds, the chemistry never had a chance to kill the organisms. The EPA registers specific antimicrobial products effective against S. aureus (including MRSA strains), and their labels specify minimum concentrations and contact times that must be followed for efficacy to be guaranteed.
S. aureus also shows notable tolerance to drying compared to gram-negative bacteria. It can survive on dry surfaces for hours to days, which is why contaminated surfaces that look clean and dry can still harbor viable organisms. Regular cleaning with an appropriate disinfectant at the correct contact time is not optional if you are managing a genuine contamination risk.
What this means for food safety specifically

Staphylococcal food poisoning works differently from most other foodborne illnesses. The bacteria grow in food and produce a preformed enterotoxin. By the time the food is eaten, the toxin is already there. Even if you cook the food after contamination and kill all the bacteria, the toxin is heat-stable and can still make people sick. This is why contaminated food may look, smell, and taste completely normal, and it is also why the standard 'when in doubt, throw it out' advice for spoiled-smelling food does not cover you here.
Symptoms of staphylococcal food poisoning come on fast, typically one to six hours after eating, because the toxin is already present and does not need time to multiply in the gut. Nausea, vomiting, and stomach cramps are the hallmarks.
The most effective prevention strategies come down to three things: keeping hands clean (since nasal carriers who handle food can transfer S. aureus directly), keeping food out of the danger zone (40°F to 140°F), and not allowing food to sit at room temperature for more than two hours. The bacteria need time and the right temperature to multiply enough to produce dangerous levels of toxin. Deny them both.
| Factor | S. aureus Growth Range | Practical Implication |
|---|---|---|
| Temperature | 7°C to 48°C (optimum 37°C) | Room-temperature food is in the growth range; refrigerator temps below 7°C inhibit growth |
| pH | 4.5 to 9.3 (optimum ~7.0) | Mild acidity alone does not prevent growth; need pH well below 4.5 |
| Water activity (aw) | ~0.86 to 0.99 (optimum ~0.99) | Low-moisture foods not automatically safe; staph tolerates drying better than many pathogens |
| Oxygen | Grows with or without (facultative anaerobe) | Vacuum-packed or oxygen-limited food/surfaces are not protected from growth |
When it is a medical issue vs. a cleaning or food safety issue
If your concern is a surface, equipment, or food handling question, the answer is in the environmental controls above: temperature management, proper disinfection with appropriate contact time, and handwashing. You do not need a doctor for that.
But if you are looking at a wound or skin lesion, here is how to think about when it crosses into needing medical attention. Seek care promptly if any of the following are present:
- Fever or chills alongside a wound or skin infection
- A wound that has not improved within 48 hours of home care
- Significant pain, redness spreading beyond the wound edge, or red streaking
- A boil or abscess that is large, getting worse, or located on the face or spine
- Any sign of infection in someone who is immunocompromised, diabetic, or on immunosuppressive medications
Staphylococcal infections can escalate to sepsis faster than people expect. A boil that drains and heals without fever is often manageable, but any infection showing systemic signs needs professional evaluation. Do not wait it out if the picture is changing for the worse.
For food poisoning specifically: most cases resolve on their own within 24 to 48 hours with fluids and rest. Seek medical help if symptoms are severe, if vomiting prevents keeping any fluids down, or if the affected person is elderly, very young, or already in poor health.
A note on related organisms and antibiotic resistance
Staphylococci belong to the broader class of round bacteria that grow in clusters (cocci arranged in grape-like groupings), which is one of the first things that distinguishes them visually under a microscope. This structural detail is not just academic. It directly informs how clinical labs identify these organisms and decide on treatment.
MRSA (methicillin-resistant S. aureus) carries all the same growth characteristics described above, with the added complication that many standard antibiotics no longer work against it. Its environmental persistence, biofilm-forming ability, and nasal carriage patterns are essentially the same as susceptible S. aureus strains. The resistance is about treatment, not about where or how fast it grows.
Interestingly, the history of staphylococcal treatment is connected to antibiotic discovery. Penicillin was originally identified as a substance that kills bacteria like staphylococci, and understanding where penicillin grows naturally helps explain how early researchers stumbled onto its antibacterial properties in the first place. For anyone curious about the full arc from mold contamination to clinical antibiotic, it is worth exploring whether penicillin grows on bread, which it can under the right conditions, as that was part of the historical context around Penicillium mold research.
The bottom line: staphylococci are adaptable, persistent, and widespread, but they are not unmanageable. Temperature control, proper disinfection technique, and handwashing address the vast majority of food safety and surface contamination risks. For skin infections, matching the severity of the response to the severity of the symptoms keeps you from both underreacting and overreacting.
FAQ
Are all staphylococci “pus-forming,” or can coagulase-negative species still cause infections?
Yes. Coagulase-negative staphylococci can still cause infections, but they’re less likely to produce the classic pus-filled abscess pattern described for S. aureus. They more often show up in low-grade skin infections and, especially, device-related problems where bacteria can attach and form biofilms.
When does a boil or draining skin lesion require urgent care versus home care?
If a boil is draining and you can keep it clean and covered, it doesn’t always require urgent care immediately. However, if redness is spreading, pain is worsening, you develop fever, or you see red streaking, that suggests deeper involvement or systemic spread and you should seek medical evaluation rather than waiting for it to improve.
If I cook leftovers that may have been contaminated with S. aureus, will that prevent staphylococcal food poisoning?
Cooking after contamination may kill the bacteria but will not reliably prevent staphylococcal food poisoning if toxin has already formed. A key practical rule is prevention during holding and storage, not relying on reheating to fix a time-temperature mistake.
How should I think about the “danger zone” if the food never looks spoiled?
“Danger zone” timing is practical for food, but the more specific issue is both temperature and time. Even if food doesn’t feel hot, leaving protein-rich foods like mayonnaise-based salads, cream-filled pastries, or deli meats at room temperature for more than about two hours increases risk.
What’s the most common way people prevent staph spread on food handling but still end up with contamination?
Handwashing helps reduce transfer from a person’s nasal or skin colonization to food, but it can fail if people contaminate surfaces first and then handle food again. In practice, pairing hand hygiene with avoiding touching face, wearing gloves appropriately, and cleaning high-touch food prep areas reduces “back-and-forth” contamination.
Why can surfaces look clean but still pose a staph risk?
Yes. Staphylococci can persist on surfaces long enough to matter, and biofilms can protect cells from routine wiping. Disinfection needs both the right product and enough dwell time, and if surfaces dry immediately after spraying, the organisms may survive.
If someone keeps getting staph skin infections, should they be checked for nasal carriage?
Not always. If you’re seeing persistent symptoms, frequent recurrences, or infections that seem to worsen quickly, clinicians may evaluate for risk factors like nasal carriage, skin conditions that disrupt the barrier, and household transmission patterns.
Does staph cleaning change for dry surfaces like stainless steel or plastic?
Dry-surface biofilms can be more resistant than moist forms, so standard “spray and wipe fast” cleaning may underperform. Make sure the cleaning/disinfectant is compatible with the surface, use the correct concentration, and keep the surface wet for the full label contact time.
If it’s MRSA, does it behave differently in food or on surfaces than regular S. aureus?
MRSA is distinguished by antibiotic resistance, not by different growth conditions or a different typical habitat. It can colonize similarly and survive on surfaces and in biofilms in the same broad ways, so prevention focuses on the same hygiene, temperature control, and correct disinfection.
What should I do if I suspect an abscess rather than a simple irritation or minor rash?
If symptoms suggest abscess formation, supportive care is not the same as treatment. Incision and drainage (when appropriate) plus clinician-directed decisions about antibiotics can be important, especially if there’s spreading redness, systemic symptoms, or locations that are high risk.
For staphylococcal food poisoning, when is “wait it out” not the right choice?
If symptoms are severe (for example, persistent vomiting, signs of dehydration, or bloody diarrhea), prompt medical assessment is safer. Also seek help sooner for infants, older adults, pregnant people, and those with chronic illness, since dehydration and complications can develop faster.
Can Bacteria Grow in Vinegar? pH, Survival, and Safety Tips
Explore if bacteria can grow in vinegar, how pH and dilution affect survival, and practical food-safety storage tips.


